Heading 2
Lorem ipsum dolor sit amet, consectetur adipisicing elit. Nostrum minus ea suscipit porro alias corporis libero at. Perferendis omnis, veniam nemo beatae vel? Tempora numquam a repellat eaque natus, magnam?
Heading 2
Lorem ipsum dolor sit amet, consectetur adipisicing elit. Autem ipsum mollitia neque, illum illo excepturi, eum incidunt fugit nostrum est, voluptate eaque minima corporis debitis at, dolores ipsam. Quaerat, dolores.
Heading 2
Lorem ipsum dolor sit amet, consectetur adipisicing elit. Autem ipsum mollitia neque, illum illo excepturi, eum incidunt fugit nostrum est, voluptate eaque minima corporis debitis at, dolores ipsam. Quaerat, dolores.
Heading 2
Lorem ipsum dolor sit amet, consectetur adipisicing elit. Autem ipsum mollitia neque, illum illo excepturi, eum incidunt fugit nostrum est, voluptate eaque minima corporis debitis at, dolores ipsam. Quaerat, dolores.
Heading 2
Lorem ipsum dolor sit amet, consectetur adipisicing elit. Autem ipsum mollitia neque, illum illo excepturi, eum incidunt fugit nostrum est, voluptate eaque minima corporis debitis at, dolores ipsam. Quaerat, dolores.
Radiant, camera-ready skin for your wedding day requires careful planning and the right professional guidance well before you say “I do.”
Starting your skin journey early gives treatments time to work, allows for adjustments, and prevents the stress of dealing with unexpected reactions close to your big day. Here’s exactly when to schedule each treatment for the best possible results!
12-6 Months Before the Wedding
This early window opens the door for transformative treatments that need significant recovery time. Schedule your initial consultation with a dermatologist at Calkin & Boudreaux to discuss your specific concerns and create a personalized plan.
Fraxel Dual Laser
Deep wrinkles, acne scars, and rough texture require this powerful resurfacing treatment. Fraxel works by creating microscopic wounds that trigger your skin to produce fresh, healthy cells.
Recovery takes one to two weeks per session, and most brides need three to four treatments for dramatic improvement. Starting now gives each session time to heal completely while allowing your skin to rebuild collagen between appointments.
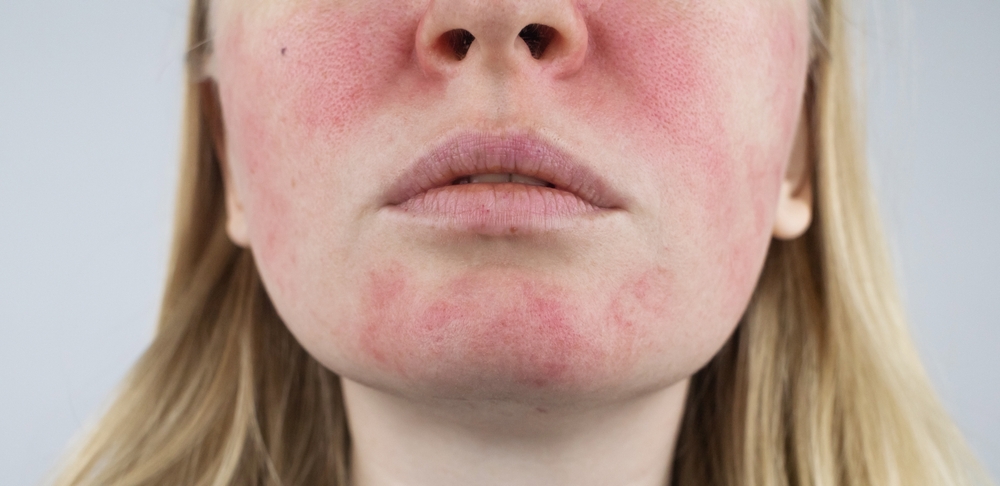
Prescription Treatments for Acne

Persistent breakouts won’t clear up overnight. Prescription medications like retinoids or oral antibiotics often take three to six months to show their full effects. Beginning treatment early prevents the panic of dealing with active acne as your wedding approaches. Your dermatologist can adjust medications if the first option doesn’t work, something impossible to do in a shorter timeframe.
Medical-Grade Skincare Foundation
Building a solid routine now sets the stage for every treatment that follows. Professional-strength products with ingredients like vitamin C, hyaluronic acid, and prescription retinoids improve your baseline skin quality.
Consistency matters more than quick fixes. Daily use of the right products gradually fades hyperpigmentation, strengthens your skin barrier, and creates the healthy canvas that makes all other treatments more effective.
6-3 Months Before the Wedding
The middle months focus on refinement and addressing specific concerns without the lengthy recovery of more aggressive options.
Chemical Peels for Brightness and Texture
Dull skin, uneven tone, and minor texture issues respond beautifully to a series of chemical peels. These controlled exfoliation treatments remove dead surface cells and reveal the fresh, glowing skin underneath.
Multiple sessions spaced four to six weeks apart build cumulative results. Starting in this window gives you time for three peels, which creates noticeable improvement without overwhelming your skin.
IPL FotoFacial for Sun Damage
Brown spots, broken capillaries, and overall redness show up harshly in wedding photos. IPL FotoFacial uses light energy to target these pigmentation and vascular issues. You’ll need two to three treatments for significant clearing, with each session spaced about one month apart. Some darkening of spots occurs before they flake off, which is why timing matters.
Emily McKenzie, MD, a board-certified dermatologist at Golden State Dermatology in Alamo, explains the importance of this mid-timeline phase:
“Many brides want to rush into injectables without addressing skin quality first. The most stunning wedding day results come from improving the canvas before adding enhancements. When we tackle texture, tone, and overall skin health in these middle months, any final touches with fillers or Botox look that much more natural and beautiful.”
Microneedling for Scars and Firmness
Acne scars, enlarged pores, and loss of firmness improve dramatically with microneedling. Tiny needles create controlled micro-injuries that trigger collagen production and skin renewal. Plan for three to four sessions spaced four to six weeks apart. Results build gradually as your skin produces new collagen, with continued improvement for several months after your final treatment.
Trial Run for Botox
First-time Botox should never happen close to your wedding. Testing it at the six-month mark shows you exactly how your face responds and whether you like the look.
Some people bruise easily or feel the results are too strong or too subtle. Knowing your response now prevents wedding day regrets and allows adjustments to your final pre-wedding appointment.
3-1 Months Before the Wedding
Final enhancement treatments happen during this window when your skin has already improved significantly. Choose based on your remaining goals.
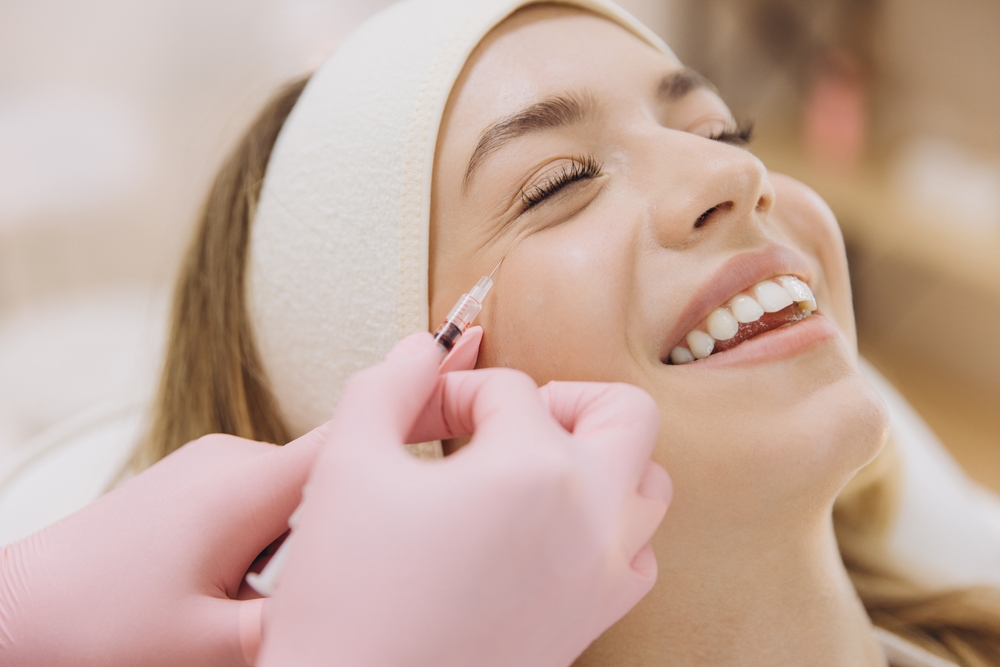
Dermal Fillers for Volume and Smoothness
These gel-based injections add subtle volume that looks natural and photographs beautifully. Schedule filler appointments six to eight weeks before your wedding. This timing allows any swelling or bruising to resolve completely while giving you a window for minor adjustments if needed.
Botox for Line Smoothing
Book your appointment six to eight weeks out. Botox takes about two weeks to reach its full effect and lasts three to four months, putting you at peak results on your wedding day.
Maintenance Chemical Peels
If you’ve been doing peels in previous months, one final treatment about six weeks before your wedding maintains your glow. Stick with the same strength and type you’ve used successfully before.
HydraFacial or DiamondGlow
These hydrating, exfoliating treatments deliver instant radiance with zero downtime. Perfect for brides who want professional-level results without any risk of adverse reactions.
Schedule one treatment in this window, then another closer to your wedding. The immediate glow makes these ideal for brides who haven’t done more aggressive treatments throughout their timeline.
2-4 Weeks Before the Wedding
Conservative choices protect you during this critical period. This is not the time for anything new or aggressive.
Your proven skincare products should stay exactly as they’ve been for months. Resist the temptation to try that new serum your friend raves about or switch to a different moisturizer.
Ashley Kim, PA-C, a board-certified dermatologist at Dermatology & Laser Centre, a Golden State Dermatology affiliate in Studio City, advises caution during this window:
“The biggest mistake brides make is panicking about a small imperfection and trying something drastic in the final weeks. I’ve seen brides attempt aggressive peels or new acne treatments days before their wedding, only to end up with angry, inflamed skin. Trust the process you’ve been following and resist the urge to make last-minute changes.”
Your skin knows these products and responds predictably. Introducing new ingredients risks allergic reactions, breakouts, or irritation that won’t have time to heal.
Gentle Esthetician Facials
Maintaining your glow without risk requires sticking to gentle, hydrating facials with an esthetician you trust. Book your facial at least two weeks before the wedding, never closer. Even gentle treatments can occasionally cause temporary redness or minor breakouts as your skin adjusts.
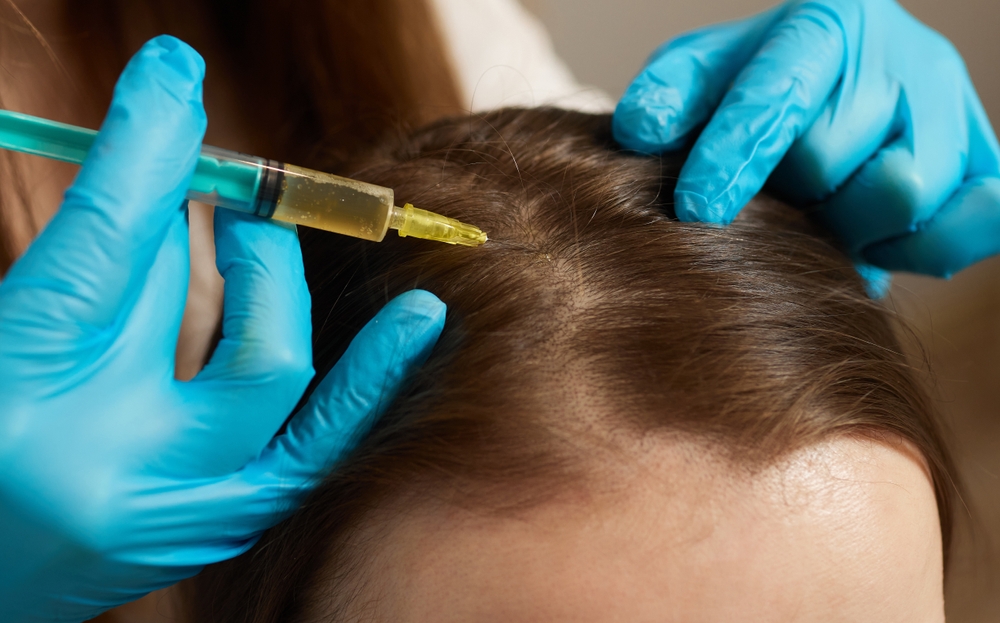
Final Laser Hair Removal
If you’ve been doing a laser hair removal series, your last session should happen at the two-week mark minimum. This gives any redness or irritation time to resolve completely.
Areas that will show in your dress, like arms, legs, or back, need this buffer period. Showing up to your wedding with inflamed skin from a too-recent treatment creates unnecessary stress.
The Week of Your Wedding
Final preparations emphasize maintaining what you’ve built rather than making changes. Simple, proven treatments keep you glowing without any risk.
Optional Gentle Facial
Schedule a calming, hydrating facial three to four days before your wedding if you want professional pampering. Choose only treatments you’ve had before with an esthetician who knows your skin.
Skip this entirely if you’re nervous about any reaction. Your at-home routine will keep you looking great, and the peace of mind might be worth more than the treatment.
Emergency Spot Treatments

Unexpected blemishes sometimes appear despite your best efforts. Your dermatologist can provide cortisone injections for particularly stubborn spots that pop up in the final days.
Call your dermatologist’s office as soon as you notice a problem spot. Quick treatment can minimize the issue significantly, but you need professional help rather than attempting aggressive at-home extraction.
Daily Routine Maintenance
Continue your established morning and evening skincare exactly as you have been. This consistency keeps your skin balanced and prevents any last-minute surprises.
Stay hydrated, prioritize sleep when possible, and limit alcohol consumption. These lifestyle factors impact how your skin looks and photographs more than most people realize.
Start Your Journey to Wedding Day Radiance
The difference between hoping for great skin and actually having it comes down to planning and professional guidance. Brides who start early and follow a strategic timeline walk down the aisle with genuine confidence.
If you have questions about your skin, schedule an appointment at Calkin & Boudreaux today!